9 am to 8 pm
Protect Your Vision from Diabetes

35+
Years
2
Hospitals
10+
Eye Specialists

30K+
Eye Surgery Treated

What is Diabetic Retinopathy?
Diabetic retinopathy is an eye condition caused by prolonged high blood sugar levels that damage the tiny blood vessels of the retina. Over time, these damaged vessels may leak, swell, or close off, affecting the retina’s ability to produce clear images.
If not detected and treated early, diabetic retinopathy can lead to blurred vision, significant vision loss, and advanced cases, permanent blindness. Since the condition often develops without noticeable symptoms in its early stages, regular eye examinations are essential for all people with diabetes.
Treatment for Diabetic Retinopathy
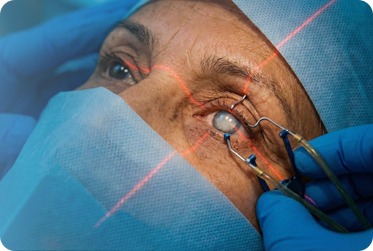
Treatment depends on the stage and severity of the disease. Early detection allows timely intervention, which can slow progression and prevent serious vision loss. Treatment options may include laser therapy, intravitreal injections, or advanced retinal surgical procedures to control leakage, reduce swelling, and protect vision.

Blurred or fluctuating vision

Small dark spots, floaters, or lines in the field of vision

Difficulty reading or seeing at night

Colours appearing faded or washed out

Sudden vision loss in the advanced stages
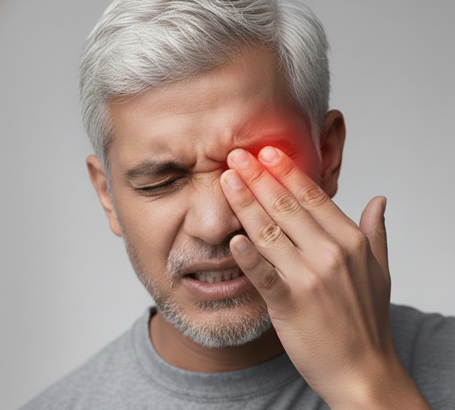
Eye discomfort or pressure (usually in advanced complications)
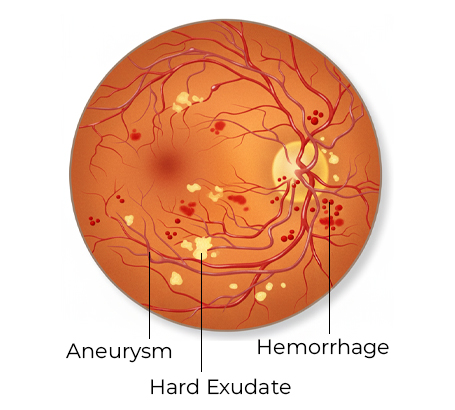
Non-Proliferative Diabetic Retinopathy (NPDR) The early stage of the disease, where weakened retinal blood vessels leak fluid or blood, gradually affects vision.
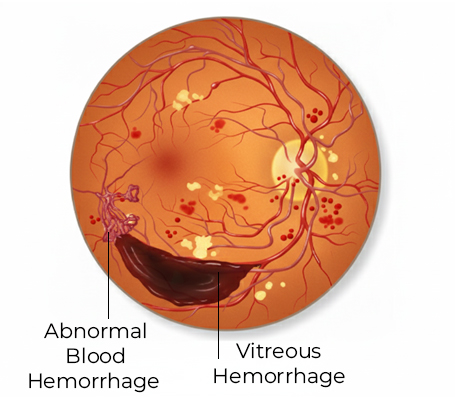
Proliferative Diabetic Retinopathy (PDR) An advanced stage where abnormal new blood vessels grow on the retina, increasing the risk of bleeding, retinal detachment, and rapid vision loss.
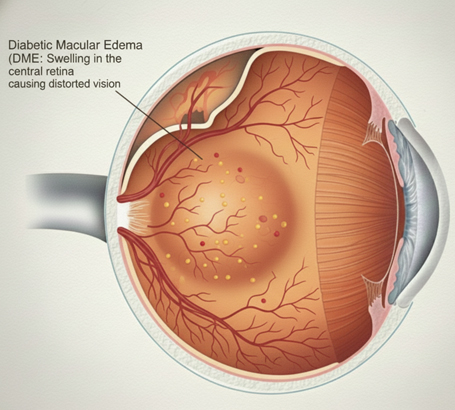
Diabetic Macular Edema (DME) Swelling of the macula (the central part of the retina), leading to blurred or distorted central vision. DME can occur at any stage of diabetic retinopathy.
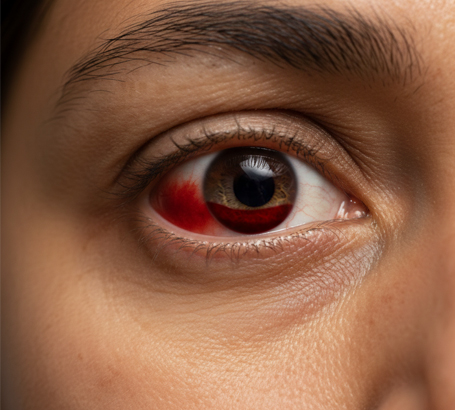
Vitreous hemorrhage Bleeding into the clear gel inside the eye, causing sudden vision loss.
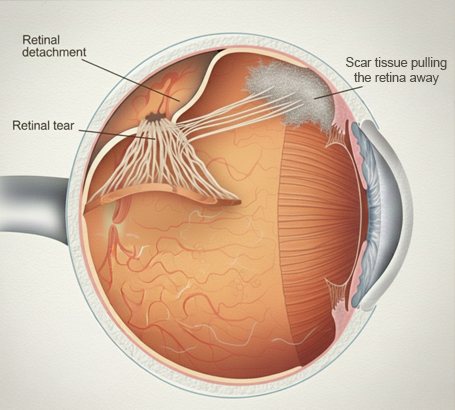
Scar tissue pulls the retina away from its normal position, leading to severe vision impairment.
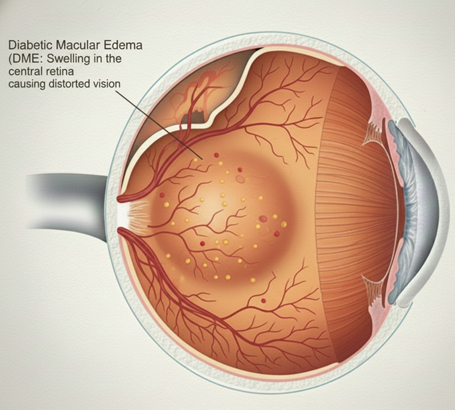
Swelling of the macula (the central part of the retina), leading to blurred or distorted central vision. DME can occur at any stage of diabetic retinopathy.

Neovascular glaucomaAbnormal blood vessels block fluid drainage, increasing eye pressure and damaging the optic nerve.

Permanent blindnessLong-standing, untreated diabetic retinopathy can result in irreversible damage.
Treatment Options for Diabetic Retinopathy
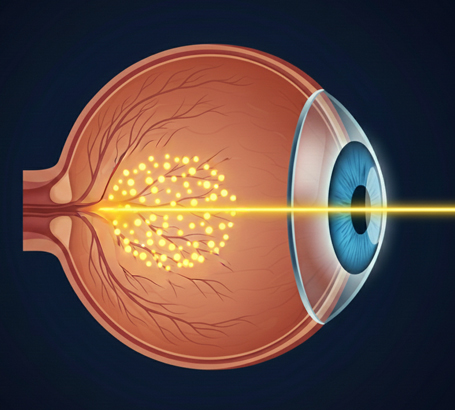
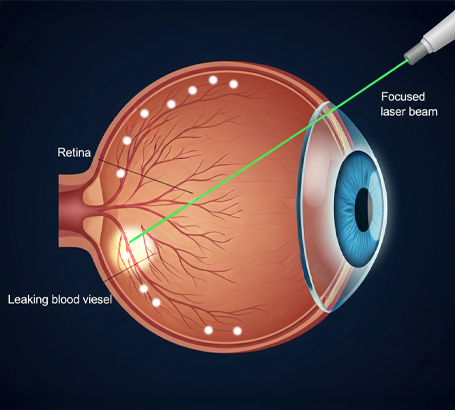
Laser Photocoagulation:
A precise laser treatment that seals leaking blood vessels and prevents further retinal damage.
Optimal Blood Sugar, Blood Pressure & Cholesterol Control
Effective diabetes and systemic health management significantly slows disease progression.
Intravitreal Injections
Safe, well-tolerated anti-VEGF or steroid injections reduce retinal swelling and inhibit abnormal vessel growth.
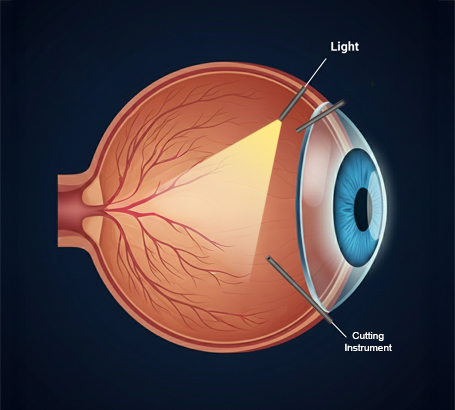
Vitrectomy surgery
A specialised surgical procedure to remove blood, scar tissue, or traction from within the eye in advanced cases.
Why Choose ASG Narang Eye Institute
ASG Narang Eye Institute offers world-class cataract surgery powered by advanced laser platforms, detailed corneal mapping, and personalized vision planning. With expert surgeons, a strict safety-first approach, and easy EMI options, patients enjoy sharper vision, fast recovery, and the freedom from glasses with high precision and comfort.
Advanced technologies for Diabetic Retinopathy management at ASG
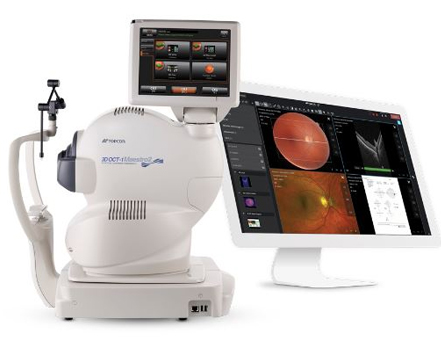
Anterior Segment OCT
High-resolution cross-sectional imaging of the cornea and surrounding structures.
-
Non-invasive imaging
-
Detects early structural changes
-
Monitors disease progression
-
Guides surgical planning
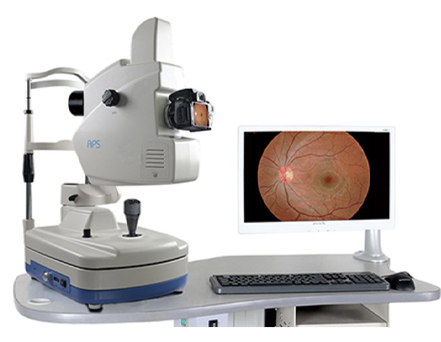
FFA
A dye-based test that shows leakage and blockages in retinal vessels.
-
Dye-based test to identify leakage and blocked blood vessels
-
Maps retinal damage precisely
-
Essential for treatment planning in advanced cases
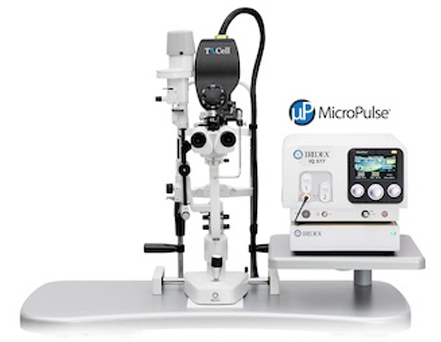
Retinal Laser System
Safe, targeted laser that seals leaks and prevents further damage.
-
Quick outpatient procedure
-
Protects remaining vision
-
Stops disease progression
Your Step-by-Step Diabetic Retinopathy Care Journey
- Comprehensive retinal examination
- OCT and angiography if required
- Detailed discussion of diagnosis and treatment options
Consultation
1
- Selection of the most appropriate treatment
- Guidance on diabetes and systemic health control
- Clear explanation of timelines and expectations
Treatment Planning
2
- Quick outpatient procedures
- Advanced retinal technology
- High safety standards with minimal discomfort
Treatment
3
- Regular retinal monitoring
- Treatment adjustments based on disease progression
- Long-term protection against vision loss
Follow-up & Maintenance
4
- Comprehensive eye exam
- Discussing lifestyle needs and lens options.
- Personalized treatment plan
Consultation
1
- Detailed pre-surgery checks
- Guidance on medications as needed.
- Step by step surgery walkthrough.
Preparation
2
- Quick, painless outpatient surgery (15 mins).
- Advanced phaco or laser-assisted techniques.
- Placement of your chosen intraocular lens (IOL).
Surgery
3
- Return to daily activities with minimal downtime.
- Mild sensitivity as vision sharpens.
- Follow-ups to ensure smooth recovery
Recovery
4
Patient Experiences
Clear Answers for Better Vision
What is diabetic retinopathy?
Diabetic retinopathy is a complication of diabetes that affects the eyes. It is caused by damage to the tiny blood vessels in the retina—the light-sensitive tissue at the back of the eye. If left untreated, it can lead to severe vision loss or permanent blindness.
What causes this condition?
Consistently high blood sugar levels damage the retinal blood vessels over time. These vessels may swell and leak fluid or close off completely, blocking blood flow. In advanced stages, the eye grows abnormal new blood vessels (proliferative retinopathy) that are fragile and prone to bleeding.
Who is at risk for developing diabetic retinopathy?
Anyone with Type 1 or Type 2 diabetes is at risk. The longer you have lived with diabetes, the higher the risk becomes. Other contributing factors include poorly controlled blood sugar, high blood pressure, high cholesterol, and pregnancy.
What are the common symptoms?
In the early stages, diabetic retinopathy often has no symptoms. As the condition progresses, you may notice:
Floating spots or dark strings (floaters).
Blurred or fluctuating vision.
Dark or empty areas in your field of vision.
Difficulty perceiving colors.
Sudden vision loss in severe cases.
How is diabetic retinopathy diagnosed at ASG Narang Eye Institute
Our specialists use a comprehensive dilated eye exam to view the retina clearly. We also utilize advanced diagnostic technology, including:
OCT (Optical Coherence Tomography): To get high-resolution cross-sectional images of the retina.
How often should diabetic patients get an eye check-up?
Early detection is vital. We recommend a dilated eye exam at least once a year, even if your vision feels perfectly normal. If retinopathy is already present, our doctors may suggest more frequent visits to monitor progression.
Is it possible to prevent diabetic retinopathy?
While you cannot always prevent it, you can significantly reduce the risk of vision loss. Proper management of blood sugar, blood pressure, and cholesterol, combined with regular eye screenings at an ASG branch, is the best way to protect your sight.
What advanced treatments are available at ASG Narang Eye Institute?
Treatment is tailored to the severity of the disease and may include:
Intravitreal Injections: Advanced medications to reduce retinal swelling.
Laser Photocoagulation: To seal leaking blood vessels and shrink abnormal ones.
Vitrectomy: A specialized surgery for advanced cases involving significant bleeding or retinal scarring.
Are the treatments painful?
No. Most treatments are performed under local anesthesia or using numbing eye drops. While you may feel a slight sensation of pressure during an injection or laser session, the procedures are generally quick and comfortable.
Can my vision be restored after treatment?
Treatment is highly effective at stopping or slowing further vision loss. In many cases, early intervention can also improve existing vision. However, because retinal tissue is delicate, the goal is to treat the condition before permanent damage occurs.
Every Angle of Vision.
Every Kind of Care.

Cataract
What do you understand by Cataract? A cataract is an eye condition characterized by the…

LASIK Surgery
What is LASIK Surgery? LASIK (Laser-Assisted In Situ Keratomileusis) or laser..
Glaucoma
What do you understand by Glaucoma? A Silent Thief of Sight Glaucoma is an eye condition…
Book Your Appointment
Submit Your Request
Get a Call from Our Team
Meet Your Specialist
Begin Your Eye Care Journey
Our Branches



